Ovarian Cysts
The ovaries are two small organs located on either side of the uterus in a woman’s body. They make hormones, including estrogen, which trigger menstruation. Every month, the ovaries release a tiny egg. The egg makes its way down the fallopian tube to potentially be fertilized. This cycle of egg release is called ovulation.
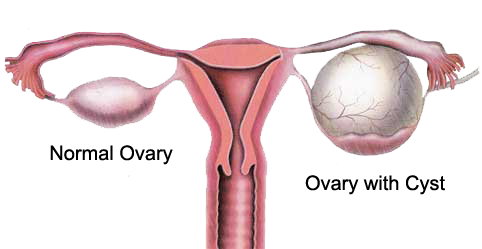 What causes ovarian cysts?
What causes ovarian cysts?
Cysts are fluid-filled sacs that can form in the ovaries. They are very common. They are particularly common during the childbearing years. There are several different types of ovarian cysts. The most common is a functional cyst. It forms during ovulation. That formation happens when either the egg is not released or the sac — follicle — in which the egg forms does not dissolve after the egg is released.
Other types of cysts include:
• Polycystic ovaries – In polycystic ovary syndrome (PCOS), the follicles in which the eggs normally mature fail to open and cysts form.
• Endometriomas – In women with endometriosis, tissue from the lining of the uterus grows in other areas of the body. This includes the ovaries. It can be very painful and can affect fertility.
• Cystadenomas – These cysts form out of cells on the surface of the ovary. They are often fluid-filled. • Dermoid cysts – This type of cyst contains tissue similar to that in other parts of the body. That includes skin, hair, and teeth. Laparoscopic removal of dermoid cysts can be done easily.
Causes ovarian tumors:
Tumors can form in the ovaries, just as they form in other parts of the body. If tumors are non-cancerous, they are said to be benign. If they are cancerous, they are called malignant. The three types of ovarian tumors are:
• Epithelial cell tumors start from the cells on the surface of the ovaries. These are the most common type of ovarian tumors. • Germ cell tumors start in the cells that produce the eggs. They can either be benign or cancerous. Most are benign.
• Stromal tumors originate in the cells that produce female hormones.
• Doctors aren’t sure what causes ovarian cancer. They have identified, though, several risk factors, including: • Age – specifically women who have gone through menopause
• Smoking
• Obesity
• Not having children or not breastfeeding (however, using birth control pills seems to lower the risk) • Taking fertility drugs (such as Clomid)
• Hormone replacement therapy
• Family or personal history of ovarian, breast, or colorectal cancer (having the BRCA gene can increase the risk)
Symptoms of ovarian cysts and tumor:
Often, ovarian cysts don’t cause any symptoms. You may not realize you have one until you visit your health care provider for a routine pelvic exam. Ovarian cysts can, however, cause problems if they twist, bleed, or rupture.
If you have any of the symptoms below, it’s important to have them checked out. That’s because they can also be symptoms of ovarian tumors. Ovarian cancer often spreads before it is detected.
Symptoms of ovarian cysts and tumors include:
• Pain or bloating in the abdomen
• Difficulty urinating, or frequent need to urinate
• Dull ache in the lower back
• Pain during sexual intercourse
• Painful menstruation and abnormal bleeding
• Weight gain
• Nausea or vomiting
• Loss of appetite, feeling full quickly
Diagnosis of Ovarian Cysts and Tumors:
Tests that look for ovarian cysts or tumors include:
• Ultrasound. This test uses sound waves to create an image of the ovaries. The image helps the doctor determine the size and location of the cyst or tumor.
• Other imaging tests. Computed tomography (CT), magnetic resonance imaging (MRI), and positron emission tomography (PET) are highly detailed imaging scans. The doctor
can use them to find ovarian tumors and see whether and how far they have spread.
• Hormone levels. The doctor may take a blood test to check levels of several hormones. These include luteinizing hormone (LH), follicle stimulating hormone (FSH), estradiol, and testosterone.
• Laparoscopy. This is a surgical procedure used to treat ovarian cysts. It uses a thin, light-tipped device inserted into your abdomen. During this surgery, the surgeon can find cysts or tumors and may remove a small piece of tissue (biopsy) to test for cancer.
• CA-125. If the doctor thinks the growth may be cancerous, he might take a blood test to look for a protein called CA-125. Levels of this protein tend to be higher in some — but not all — women with ovarian cancer. This test is mainly used in women over age 35, who are at slightly higher risk for ovarian cancer.
Treatment of Ovarian Cysts and Tumors:
Surgery is an option if the cyst doesn’t go away, grows, or causes you pain. There are two types of surgery:
1. Laparoscopy uses a very small incision and a tiny, lighted telescope-like instrument. The instrument is inserted into the abdomen to remove the cyst. Laparoscopic removal of ovarian cysts done very easily. Large size ovarian tumour can be removed laparoscopically.benign cysts are removed laparoscopically.
2. Laparotomy involves a bigger incision in the stomach. Doctors prefer this technique for larger cysts and ovarian tumors. If the growth is cancerous, the surgeon will remove as much of the tumor as possible. This is called debulking. Depending on how far the cancer has spread, the surgeon may also remove the ovaries, uterus, fallopian tubes, omentum — fatty tissue covering the intestines — and nearby lymph nodes.
3. Chemotherapy: drugs given through a vein (IV), by mouth, or directly into the abdomen to kill cancer cells. Because they kill normal cells as well as cancerous ones, chemotherapy medications can have side effects, including nausea and vomiting, hair loss, kidney damage, and increased risk of infection. These side effects should go away after the treatment is done.
Laparoscopic management of ovarian cysts:
The laparoscopic management of benign adnexal masses is well established. However, when managing ovarian cysts in postmenopausal women, it should be remembered that the main reason for operating is to exclude an ovarian malignancy. If an ovarian malignancy is present then the appropriate management in the postmenopausal woman is to perform a laparotomy and a total abdominal hysterectomy, bilateral salpingo-oophorectomy and full staging procedure. The laparoscopic approach should therefore be reserved for those women who are not eligible for non-invasive treatment but still have a relatively low risk of malignancy.Women who are at high risk of malignancy, as calculated using the risk of malignancy index, are likely to need a laparotomy and full staging procedure as their primary surgery. It’s recommended that laparoscopic management of ovarian cysts in postmenopausal women should involve oophorectomy (usually bilateral) rather than cystectomy. In a postmenopausal woman, the appropriate laparoscopic treatment for an ovarian cyst, which is not suitable for conservative management, is oophorectomy, with removal of the ovary intact in a bag without cyst rupture into the peritoneal cavity. There is the risk of cyst rupture during cystectomy and, as described above, cyst rupture into the peritoneal cavity may have an unfavourable impact on disease-free survival in the small proportion of cases with an ovarian cancer. If a malignancy is revealed during laparoscopy or subsequent histology, it’s recommended that the woman is referred to a cancer centre for further treatment. If an ovarian cancer is discovered at surgery or on histology, a subsequent full staging procedure is likely to be required. A rapid referral to a cancer centre is recommended for those women who are found to have an ovarian malignancy. Secondary surgery at a centre should be performed as quickly as feasible.
All ovarian cysts that are suspicious of malignancy in a postmenopausal woman, as indicated by a high risk of malignancy index, clinical suspicion or findings at laparoscopy, are likely to require a full laparotomy and staging procedure.following ovarian cysts are managed by laparoscopic method:
• Laparoscppic removal of dermoid cysts
• Laparoscopic removal of huge ovarian cysts
• Laparoscopic removal of twisted ovarian cysts
• Laparoscopic removal of chocolate cysts of ovary
• Laparoscopic removal of bilateral endometriomas
